Caring for Mothers with Ultrasounds, AI, and Nurse Midwives
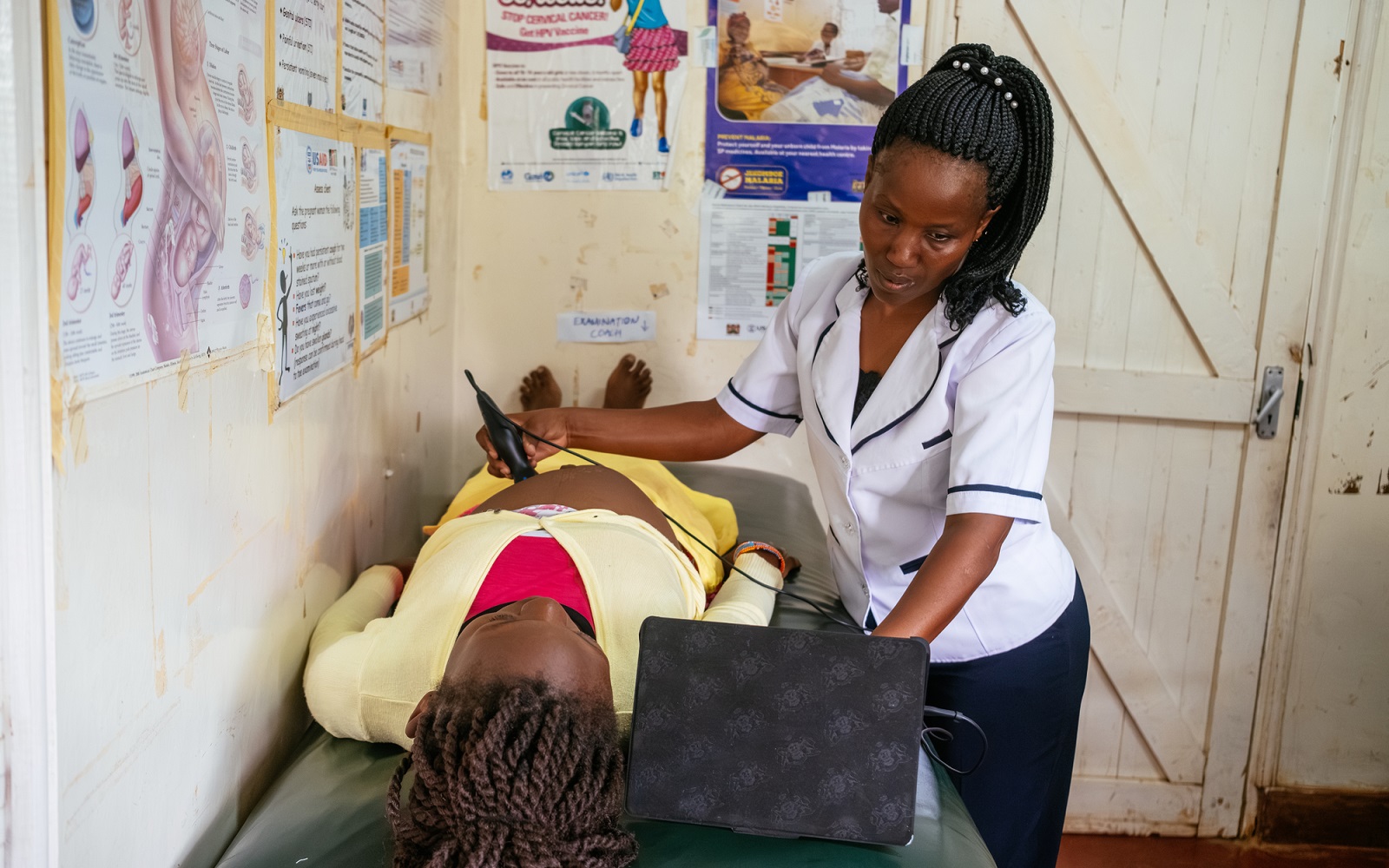
AI takes on maternal mortality
While the training takes just five days, scaling up to train tens of thousands more midwives would be a monumental task. But we’re partnering with several companies that are working on AI-enabled devices that we hope will make the technology even easier to use and require less training.
This AI involves basic machine learning. Essentially, the machines are trained with thousands of existing ultrasound images that have been reviewed and annotated by sonographers to train algorithms that identify specific risks. Midwives sweep the ultrasound probe across the woman’s belly several times while the algorithm runs in the background. After a short exam, the device can flag whether the pregnancy is high risk, and the nurse or midwife can then provide recommendations to the woman on the location, content, and frequency of care that she needs.
The algorithms are now being honed and tested in the field. So far, researchers have found that the AI does a good job identifying high-risk pregnancies. One study found that the AI-enabled devices can estimate one key data point, gestational age, with more accuracy than humans.
“It will revolutionize midwifery in this country,” Githemo says.
Dr. Beatrice Murage, director of sustainability and health equity at one company we are working with in this effort, sees ultrasounds as benefiting not only individual families but entire communities. As a doctor practicing in rural Kenya, she has lost mothers during delivery. She has seen others left with life-altering consequences after pregnancy complications—everything from debilitating depression to major surgeries and devastating fistulas.
“When a mother gets good care for her and her baby, that touches on so many of the Sustainable Development Goals: gender equity, health, poverty,” Murage says. “Bringing this kind of care closer to the mother is really an ecosystem story. The potential is really large.”
We expect to see regulatory approval for these devices in the next two years. In the meantime, our foundation and others are working on how to quickly get the device into more midwives’ hands after that.
Inspiring pregnant women to seek care earlier
When developing technology like this, the main goals include, most obviously, identifying risky pregnancies to save the lives of mothers and babies. We’re hopeful that the number will ultimately be in the millions. But patients are experiencing other benefits, too.
Veronica Fulano Nato, a nurse trained by Githemo’s team, says ultrasounds are changing the way mothers-to-be think about their pregnancies. Before, it wasn’t unusual for a pregnant woman to wait until she began labor to make her first visit Nato’s clinic in Kilifi, Kenya. That’s a problem because Nato would have to spring into action without knowing anything about the pregnancy. Were mother and baby healthy? Was the delivery high risk? If something goes wrong at the clinic, getting the woman to the hospital can take an hour. Now, women are starting to come to the clinic earlier in the pregnancy, eager to see the ultrasound images and confident they’re getting state-of-the-art care.
“They’re so happy,” Nato says. “They say, ‘It feels like we’re at a big-city hospital.’”
link







