Quality communication can improve patient-centred health outcomes among older patients: a rapid review | BMC Health Services Research

Study selection
After running the search strategy, 40 articles were identified from PubMed, 13 from Google Scholar (records identified from websites (Fig. 1)), 24 from Scopus, 18 from CINHAL, and 10 from PsycINFO based on the relevance of the titles. It was discovered that 26 were duplicated records between databases and Google Scholar, which reduced the number of identified records to 79. Further, the automation tool (ASReview) marked five records as ineligible based on their title considering the inclusion and exclusion criteria. These articles were excluded because the author confirmed in the fourth round that they were ineligible. After realising they did not focus on older adults, the author excluded three more records. Therefore, 71 records were screened using their abstracts with the help of ASReview (64 records from databases and 7 records from Google Scholar), whereby 44 were excluded (40 records from databases and 4 records from Google Scholar) for various reasons, such as being expert opinions and professional development based on field experiences (e.g., [28]) and did not have a methodology. The remaining 27 records (24 records from databases and 3 records from Google Scholar) were sought for retrieval, whereby one was excluded because its full text was inaccessible. The remaining 26 articles (23 records from databases and 3 records from Google Scholar) were assessed for eligibility with the help of ASReview, whereby eight records were excluded because they did not report their methodologies (e.g., [29]), another eight were secondary studies (e.g., [30]), and three were non-peer-reviewed preprints. Therefore, seven studies met the eligibility criteria for this rapid review.
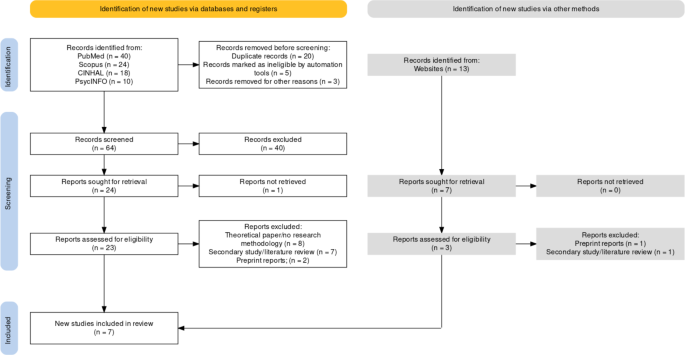
PRISMA Flowchart summarising the study selection process
Study characteristics
Out of the seven studies, one was an experimental study [31], one was a cross-sectional observational study [32], and five were qualitative studies [33,34,35,36,37]. As shown in Table 3, most of the studies (n = 4) were conducted in the United States. The following countries produced one study each: Australia, Cameroon, the Netherlands, and Hungary. Although all the studies utilised a sample of older patients, the characteristics of the patients differed from one study to another. The studies ranged from primary care settings [36] and adult medical wards [37] to long-term care facilities like nursing homes. Apart from [36], the rest of the studies investigated various non-verbal communication strategies with older adults and their impact on various types of patient-centred outcomes, ranging from health-related outcomes (e.g., smoking cessation) to patient-reported outcomes, such as patient satisfaction, self-esteem, and life satisfaction. These outcomes are within the broader umbrella category of patient-centred m outcomes.
Further, the studies used different types of communicative strategies that can be used to enhance or promote patient-centred outcomes. In this rapid review, they were categorised into seven, namely (a) touching, (b) smiling, (c) gaze, head nod, and eyebrow movement, (d) active listening, (e) close physical distance, and (f) use of visual aids, and (g) telephone communication. Table 4 summarises the various ways in which each study described its interventions.
Quality assessment findings
All seven studies were of high quality based on the GRADE Tool-based Assessment. However, [31] conducted an experimental study, but they did not provide any details indicating whether there was concealment in participant allocation and blinding of participants and outcome assessors. Therefore, it has a high likelihood of risk of bias. However, they scored excellently in the other domains of the GRADE Tool. All five qualitative studies and the cross-sectional observational study also scored excellently in the domains of the GRADE Tool, apart from the imprecision domain where they could not be scored because none of them reported effect sizes (Table 5).
Results of individual studies
[31] was the only experimental study used in this rapid review investigating the effect of comfort touch on older patients’ perceptions of well-being, self-esteem, health status, social processes, life satisfaction, self-actualisation, and self-responsibility. The authors did not report the effect sizes but indicated that comforting touch had a statistically significant effect on each of the five variables. In summary, the authors suggested that comfort touch, characterised by a handshake or a pat on the shoulders, forearm, or hand, had a statistically significant positive impact on the various patient-centred outcomes reported in their study. For each variable, the authors used three groups, the first and second control groups and the third experimental group. After delivering the intervention, they investigated whether the scores of these variables changed between three-time points in each of the three groups. The first time point was the baseline data collected before intervention was initiated; the second was two weeks after baseline data; and the third was four weeks after baseline data. The authors found that in each of the five variables, the scores remained almost the same in the three-time points for the two control groups, but there were significant improvements in the experimental group (the one that received the intervention). For example, the self-esteem variable was measured using Rosenberg’s Self-Esteem Scale, with the highest attainable score of 40. In the first control group, the score remained 27.00, 27.27, and 27.13 for Time 1 (baseline), Time 2 (after two weeks), and Time 3 (after four weeks), respectively. The same trend was observed in the second control group. However, in the experimental group, the score improved from 29.17 at baseline to 36.00 at Time 2 and 37.47 at Time 3. These findings suggest that comfort touch was highly effective in improving self-esteem among older patients. The same significant improvements were evident for all the other variables (p.184).
While all the other studies focused on nonverbal communication cues, [36] focused on telephone communication. They aimed to investigate the effect of a tailored intervention on health behaviour change in older adults delivered through telephone communication. Therefore, the primary rationale for selecting this study for review is that it used a specific communicative strategy (telephone) to deliver the intervention, which is the primary purpose of effective communication in most healthcare settings. The older patients used as participants in this study lived with COPD. The nurses trained to administer the intervention made regular phone calls over 12 months. The intervention was delivered to 90 participants. Of these, 65 were invited for interviews at the end of 12 months. One of the most important outcomes relevant to this rapid review is that the participants reported “being listened to by a caring health professional.“ It means that regular telephone communication improved the patient’s perceptions of the quality of care. Other critical patient-centred outcomes that improved due to this intervention include many participants quitting smoking and increased awareness of COPD effects.
[34] also conducted a qualitative study but needed to specify the specific research design, which was generally non-experimental. The authors used formative evaluation and a participatory approach to develop a communicative intervention for older adults with limited health literacy. In other words, apart from literature reviews, the authors involved the target population in developing a curated story to improve their health literacy. They developed photo and video-based stories by incorporating narrative and social learning theories. The most important finding of this study was that the authors found the developed communicative strategy appealing and understandable. Such observations imply that the participants’ health literacy also likely improved even though the authors did not evaluate it.
Further, using a sample of 155 older patients, [32] investigated the relationship between the communication characteristics between nursing practitioners and the older patients and patients’ proximal outcomes, namely patient satisfaction and intention to adhere to the NPs’ recommendations, and patients’ long-term outcomes (presenting problems and physical and mental health). The proximal outcomes (satisfaction and intention to adhere) were measured after visits, whereas the long-term outcomes (presenting problems, mental health, and physical health) were measured at four weeks. The communication and relationship components observed include various non-verbal communication strategies: smile, gaze, touch, eyebrow movement, head nod, and handshakes. The authors recorded videos during patient-provider interactions. These communicative strategies were measured using the Roter Interaction Analysis System (independent variable).
In contrast, the other outcomes (dependent variables) outlined above were each measured separately with a validated tool or single-item instruments [32]. For example, presenting problems were measured with a single-item instrument, whereas the physical and mental health changes at four weeks were measured using the SF-12 Version 2 Health Survey. The authors found that verbal and nonverbal communication strategies focused on providing patients with biomedical and psychosocial information and positive talk characterised by receptivity and trust were associated with better patient outcomes, such as significant improvements in mental and physical health at four weeks. Although the study did not report effect sizes, the findings agree that effective and quality communication can improve patient-centred outcomes like patient satisfaction.
[35] conducted a qualitative study with focus groups (eight focus groups with a range of three to nine participants) of 15 older adults in a nursing home. The study used an ethnographic qualitative design. The nonverbal communication strategies observed in this study included active listening (including verbal responses) and touching. The authors found that the characteristics of the communication strategies that make communication quality and effective include mutual respect, equity, and addressing conflict. The patients perceived that their nursing aides gave them better-individualised care if their relationship and communication were characterised by mutual respect. Portraying mutual respect includes showing the patients that they are being listened to and heard, which can include calling them by their names and showing signs of active listening. Some residents (older patients) complained that some nursing aides had favouritism, whereby they liked some patients and not others. When such a perception emerges, the patients could perceive the treatment as unjust, compromising individualised care quality. Also, nursing aides must equip themselves with communicative strategies to address conflict rather than avoid it. For example, knowing about the patient’s history can help nursing aides understand their behaviour in the facility, improving prospects of providing better personalised or individualised care.
[33] also conducted a qualitative study utilising a sample of 17 older adults in nursing homes and assisted living facilities in the United States. They aimed to identify the types and examples of nurse-aide-initiated communication with long-term care residents during mealtime assistance in the context of the residents’ responses. Using a naturalistic approach, the researchers observed communicative interactions between the nurse aides and the residents during mealtime assistance. Videos were recorded and transcribed and analysed using the grounded theory approach. They found that apart from emotional support, nonverbal communication strategies were used by nurse aides to address the residents, initiate and maintain personal conversations, and check-in. Although the authors did not provide statistical proof that these communication strategies improved well-being, their findings can inform future studies.
Finally, [37] conducted a qualitative, grounded theory study to develop a model for effective non-verbal communication between nurses and older patients. The authors conducted overt observations of patient-nurse interactions using a sample of eight older patients. They found that the nature of nonverbal communication to be employed depends on the context or environment, and certain external factors influence it. The factors influencing nonverbal communication include the nurses’ intrinsic factors, positive views of older adults, awareness of nonverbal communication, and possession of nonverbal communication skills. Patient factors that can also influence the effectiveness of nonverbal communication include positive moods, financial situations, and non-critical medical conditions. The model developed also emphasised that non-verbal communication, if carried out correctly considering context and environment, can lead to positive outcomes, such as increased adherence to providers’ recommendations, improved quality of care, and shorter hospital stays.
Results of syntheses
Four themes emerged from the narrative synthesis: nonverbal communication, verbal communication, communication strategies, and patient-centred outcomes. Table 6 summarises the subthemes that emerged under each theme. They are discussed below.
Nonverbal communication
Nonverbal communication was a critical theme that emerged in several studies. Five out of the seven studies investigated the effectiveness of touch on various patient-centred outcomes [31]. found that nonverbal communication strategies such as comfort touch, characterised by a handshake or a pat on the shoulders, forearm, or hand, had a statistically significant positive impact on patient-centred outcomes, such as well-being, self-esteem, health status, social processes, life satisfaction, self-actualisation, and self-responsibility [31]. implemented comfort touch exclusively without combining it with other nonverbal communication strategies. It means that comfort touch on its own can be effective in improving various patient-centred outcomes. As such, it can be hypothesised that if comfort touch is combined with other nonverbal communication strategies, such as active listening, eye gazing, smiling, maintaining a close distance, eyebrow movement, and nodding/shaking of the head can lead to even better results regarding patient-centred outcomes [32, 33, 35, 37]. [35] identified active listening and touching as important nonverbal communication strategies that make communication quality and effective [33]. found that nurse-aide-initiated communication during mealtime assistance using nonverbal communication strategies, such as emotional support, smiling, laughing, touching, eye gazing, shaking hands, head nodding, leaning forward, and a soft tone were crucial in addressing the residents, initiating (and maintaining) personal conversations, and checking in. Finally, [37] developed a model that emphasised the importance of effective nonverbal communication in forming effective therapeutic relationships, promoting patient satisfaction, and improving the quality of care. An exhaustive list of the nonverbal communication approaches is shown in Table 6.
In general, most studies, especially the qualitative ones, supported the utilisation of multiple non-verbal communication strategies in a single communicative episode. The studies also implied that it is the responsibility of healthcare providers to initiate and maintain effective nonverbal communication cues, such as those detailed in Table 6. Additionally, it is important to note that it is only one study [31] that investigated the effectiveness of comfort touch on patient-centred outcomes. Therefore, the notion implied in qualitative studies that combining various nonverbal strategies could lead to a better improvement in patient-centred outcomes is subject to further empirical investigation. It was noted that there is a lack of empirical studies investigating how the combination of various non-verbal communication techniques or strategies can influence patient-centred outcomes, such as patient satisfaction and perceptions of quality of care.
Verbal communication
Four out of the seven studies implied that verbal communication improved patient-centred outcomes [32, 34,35,36]. Effective and quality verbal communication was found to impact patient satisfaction positively [32], increased awareness of COPD effects [36], improved health literacy [34], presented problems [32], and mental and physical health [32]. It is worth noting that [32] used a cross-sectional survey approach and used regression analyses to investigate the relationship between communication and various patient-centred outcomes, such as patient satisfaction and mental and physical health. Also, it is important noting that the authors combined both verbal (e.g., more positive talk, greater trust, and receptivity) and non-verbal (e.g., smile, gazing, eyebrow movements, and interpersonal touches) in their study. Therefore, it can be a bit challenging to directly conclude that effective verbal communication alone without non-verbal communication is effective on its own in improving patient-centred outcomes. Similarly, [34] combined both narrative-based and picture-based communication strategies to give patients education about health literacy. Therefore, it can be challenging to know whether narratives comprising of verbal communication (and often non-verbal communication) can improve patient-centred outcomes on their own. The rest of the studies were qualitative [35, 36], which means that their findings generally reflected the subjective experiences or opinions of their participants. Therefore, it can be said that although all the four studies supported verbal communication can effectively improve patient-centred outcomes, there is a need for future research to experimentally test its effectiveness without being combined with non-verbal communication strategies.
Moreover, two of the four studies implied that some conditions must be met for verbal communication to be effective [32, 35]. some communication strategies, such as higher lifestyle discussion and rapport-building rates, were perceived as patronising and associated with poor outcomes [32]. Instead, the authors found that communication strategies like seeking and giving biomedical and psychosocial information were more effective in improving patient outcomes [32]. It implies that healthcare providers should be attentive and intentional of the topics they discuss with patients. Further, in their qualitative study, [35] found that effective verbal communication also requires mutual respect, equity, and addressing conflict. Indeed, it appears that certain communication strategies like lifestyle discussions can undermine the process of establishing trust, which is why they were associated with adverse patient outcomes. Also, unlike nonverbal communication, the studies that highlighted the effect of verbal communication on patient-centred outcomes did not provide rich descriptions of the specific verbal communication strategies that can be used in a face-to-face healthcare setting. The described strategies like using phone calls to regularly communicate with the patient without having to visit a healthcare facility and things to ensure when communicating with the older patient, such as mutual respect and avoiding too many discussions on lifestyle do not offer rich insights into the specific nature of the verbal communication strategies.
Communication strategies
In 3.5.2 above, it was shown that the sample of participants that [32] used in their study did not prefer discussions related with healthy lifestyles, which compromised patient-centred outcomes. Therefore, it was also important to determine the best approaches to formulate communication strategies that work. Two out of the seven studies implied how communication strategies can be formulated [34, 36] [36]. found that a tailored intervention delivered through telephone communication improved patient perceptions of the quality of care. In this regard, the authors first identified the needs of the patients to guide the development of the tailored intervention, from which they might have obtained insights into the patients’ communication preferences [34]. found a participatory approach to developing a curated story that improves health literacy appealing and understandable. The findings emphasised the need for participatory approaches when developing communication interventions for patients with varied health and social needs. Although the studies did not compare or contrast the effectiveness of participatory-based communication strategies and non-participatory-based communication strategies, their findings provide useful insights into the significance of involving patients when developing them. From their findings, it can be anticipated that a participatory approach is more likely to yield better patient-centred outcomes than non-participatory-based communication strategies.
Patient-centred outcomes
All studies reviewed highlighted patient-centred outcomes as the goal of effective communication in older patients. Patient-centred outcomes included well-being, self-esteem, health status, social processes, life satisfaction, self-actualisation, and self-responsibility (Butt, 2001), as well as patient satisfaction [32, 36], increased awareness of COPD effects [36], and improved health literacy [34]. Others included presenting problems, mental health, and physical health [32], as well as adherence to providers’ recommendations, improved quality of care, and shorter hospital stays [37]. All seven studies indicated that the various verbal and nonverbal communication approaches could improve these patient-centred outcomes. The consistency observed between the experimental study by [31], the qualitative studies, and other quantitative study designs implies the need to pay greater attention to verbal and non-verbal communication strategies used by healthcare professionals as they can directly influence numerous patient-centred outcomes. This consistency further implies that effective communication is the anchor of high-quality care, and its absence will always compromise patient-centred outcomes, such as satisfaction and health outcomes.
link








